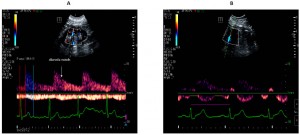
Electrocardiographic Time-Intervals Waveforms as Potential Predictors for Severe Acute Kidney Injury in Critically Ill Patients
Free full text here on the Journal of Clinical Medicine
Abstract
Background: Acute kidney injury (AKI) is common in critically ill patients admitted to intensive care units (ICU) and is frequently associated with poorer outcomes. Hence, if an indicator is available for predicting severe AKI within the first few hours of admission, management strategies can be put into place to improve outcomes. Materials and methods: This was a prospective, observational study, involving 63 critically ill patients, that aimed to explore the diagnostic accuracy of different Doppler parameters in predicting AKI in critically ill patients from a mixed ICU. Participants were enrolled at ICU admission. All underwent ultrasonographic examinations and hemodynamic assessment. Renal Doppler resistive index (RDRI), venous impedance index (VII), arterial systolic time intervals (a-STI), and venous systolic time intervals (v-STI) were measured within 2 h from ICU admission. Results: Cox proportional hazards models, including a-STI, v-STI, VII, and RDRI as independent variables, returned a-STI as the only putative predictor for the development of AKI or severe AKI. An overall statistically significant difference (p < 0.001) was observed in the Kaplan–Meier plots for cumulative AKI events between patients with a-STI higher or equal than 0.37 and for cumulative severe AKI-3 between patients with a-STI higher or equal than 0.63. As assessed by the area under the receiver operating curves (ROC) curves, a-STI performed best in diagnosing any AKI and/or severe AKI-3. Positive correlations were found between a-STI and the N-terminal brain natriuretic peptide precursor (NT-pro BNP) (ρ = 0.442, p < 0.001), the sequential organ failure assessment (SOFA) score (ρ: 0.361, p = 0.004), and baseline serum creatinine (ρ: 0.529, p < 0.001). Conclusions: Critically ill patients who developed AKI had statistically significant different a-STI (on admission to ICU), v-STI, and VII than those who did not. Moreover, a-STI was associated with the development of AKI at day 5 and provided the best diagnostic accuracy for the diagnosis of any AKI or severe AKI compared with RDRI, VII, and v-STI.